Stress is part of life. Exams, job pressure, money problems, family issues — they all affect the mind. But can stress cause seizures? Yes, stress can trigger seizures, especially in people who already have epilepsy or are prone to them.
The brain works with electrical signals. When stress increases, the body releases stress hormones like cortisol and adrenaline. These chemicals raise heart rate, increase blood pressure, and make the brain more alert. If this alert state becomes extreme, it can disturb normal brain activity. That disturbance may lead to a seizure.
Stress alone does not always create epilepsy. But it is one of the strongest seizure triggers reported by patients. Poor sleep, dehydration, anxiety, and emotional trauma often work together with stress.
This article explains everything clearly. You will learn about types of seizures, seizure symptoms, first aid, seizure diagnosis, treatment options, and risks. Let’s begin by understanding seizures in simple words.
What Are Seizures?
A seizure happens when there is sudden, abnormal electrical activity in the brain. The brain sends signals to control movement, thinking, and feeling. When those signals fire uncontrolled, the body reacts.
A seizure can affect:
- Movement
- Speech
- Awareness
- Memory
- Emotions
Some seizures cause full-body shaking. Others cause brief staring spells. Some last seconds; others last minutes.
A seizure does not always mean epilepsy. It can happen once due to fever, infection, low blood sugar, head injury, or extreme stress.
If seizures happen again and again without a clear cause, that condition is called epilepsy.
Various Types of Seizures
Seizures are grouped by where they start in the brain and how they affect awareness. Below are all major types and subtypes explained in simple medical terms.
| Seizure Type | Subtype | What Happens | Awareness | Common Age Group | Stress Connection |
|---|---|---|---|---|---|
| Focal Seizures | Focal Aware | Tingling, strange smells, sudden fear, small jerks | Fully aware | Any age | Stress and anxiety may increase episodes |
| Focal Impaired Awareness | Staring, confusion, repetitive movements | Reduced awareness | Any age | Emotional stress may increase frequency | |
| Focal to Bilateral Tonic-Clonic | Starts in one area, spreads to the full body, shaking | Loss of consciousness | Any age | Severe stress and sleep loss may trigger the spread | |
| Generalized Seizures | Tonic-Clonic | Body stiffens, then shakes | Loss of consciousness | Any age | Stress and fatigue are common triggers |
| Absence | Brief staring spell | Brief loss of awareness | Mostly children | Stress and tiredness may increase episodes | |
| Myoclonic | Sudden quick jerks | Usually aware | Teens, young adults | Sleep loss from stress increases risk | |
| Tonic | Sudden muscle stiffness | Often impaired | Children with severe epilepsy | Stress may worsen frequency | |
| Clonic | Repeated rhythmic jerking | Often impaired | Rare | Stress may act as a trigger | |
| Atonic | Sudden loss of muscle tone, sudden fall | Brief loss | Children | Poor sleep from stress may increase risk | |
| Unknown Onset | — | Start point unclear | Varies | Any age | Stress may still trigger episodes |
| Reflex Seizures | — | Triggered by flashing lights or patterns | Varies | Any age | Stress may increase brain sensitivity |
| Febrile Seizures | — | Seizure during high fever | Loss of awareness | Young children | Caused by fever, not stress |
| Psychogenic Nonepileptic Seizures (PNES) | — | Seizure-like episode without abnormal brain signals | Varies | Teens, adults | Strongly linked to emotional stress or trauma |
Seizure Symptoms
Seizures do not always look the same. Some people imagine seizures as full-body shaking, but that is only one type. In reality, seizures can affect behavior, thoughts, emotions, and the body in many different ways. The symptoms depend on which part of the brain is involved and how long the seizure lasts.
Below is a clear and simple explanation of the four main categories: behavioral, psychological, emotional, and physiological symptoms of seizure.
Behavioral Symptoms of Seizure
Behavioral symptoms are changes in actions or outward behavior during or after a seizure. These are often noticed by family members, teachers, or friends.
Common behavioral signs include:
- Sudden staring spells
- Repetitive movements (lip smacking, chewing, blinking)
- Wandering without awareness
- Sudden pause in activity
- Unusual hand movements
- Confused speech
- Acting out of character
For example, a person may suddenly stop talking and stare blankly for 10–20 seconds. In focal seizures, someone might repeatedly rub their hands or pick at clothes without knowing it.
After a seizure, behavior may change temporarily. The person may seem:
- Confused
- Irritable
- Extremely tired
- Slow to respond
These behavioral symptoms are often brief but important. They give clues about where the seizure starts in the brain.
Psychological Symptoms of Seizure
Psychological symptoms affect thinking, perception, and awareness. These symptoms may happen before, during, or after a seizure.
Common psychological symptoms include:
- Confusion
- Memory gaps
- Difficulty understanding speech
- Trouble speaking clearly
- Deja vu (feeling like something happened before)
- Jamais vu (feeling unfamiliar with known places)
- Distorted sense of time
Some people experience an aura before a seizure. An aura is actually a small focal seizure that acts as a warning. Psychological auras may include:
- Sudden fear without reason
- Feeling detached from reality
- Racing thoughts
- Strange thoughts that do not make sense
After the seizure, short-term memory loss is common. The person may not remember what happened during the episode.
Emotional Symptoms of Seizure
Seizures can strongly affect emotions because the brain areas that control emotions are often involved.
Emotional symptoms may include:
- Sudden fear
- Panic
- Anxiety
- Sadness
- Anger
- Euphoria (unusual happiness)
These emotional changes can appear suddenly and without a clear trigger.
For example, a person may suddenly feel intense fear for a few seconds before losing awareness. This is common in temporal lobe seizures.
After a seizure, emotional symptoms may continue. A person may feel:
- Depressed
- Embarrassed
- Frustrated
- Emotionally drained
In people with epilepsy, long-term emotional challenges such as anxiety or depression are more common. This is partly due to brain changes and the stress of living with seizures.
Physiological Symptoms of Seizure
Physiological symptoms are physical changes in the body caused by abnormal brain activity.
Common physical symptoms include:
- Muscle stiffness
- Jerking movements
- Shaking
- Loss of consciousness
- Rapid heartbeat
- Breathing changes
- Drooling
- Sweating
- Pale or flushed skin
In tonic-clonic seizures, the body first becomes stiff (tonic phase), then begins rhythmic jerking (clonic phase).
Other physiological signs may include:
- Tongue biting
- Loss of bladder control
- Headache after seizure
- Extreme tiredness
Some seizures only cause mild physical signs, such as:
- Eye blinking
- Facial twitching
- Slight jerking of one arm
Breathing may slow briefly during a seizure, but it usually returns to normal afterward.
Symptoms Before, During, and After a Seizure
It helps to understand seizure symptoms in three stages:
| Before (Prodrome or Aura) | During (Ictal Phase) | After (Postictal Phase) |
| Mood changes | Shaking | Confusion |
| Anxiety | Staring | Memory loss |
| Headache | Loss of awareness | Fatigue |
| Strange sensations | Repetitive movements | Emotional changes |
| Fear | Emotional outburst | Headache |
Not every person experiences all stages.
First Aid for Seizure
First aid during a seizure focuses on keeping the person safe until the episode ends. Most seizures last only a few minutes and stop on their own, but simple actions can prevent injury and complications.
- Stay calm and note the time the seizure starts.
- Protect the person from injury by moving nearby objects away.
- Place something soft under the head to prevent head injury.
- Turn the person on their side to help keep the airway clear.
- Loosen tight clothing around the neck.
- Do not put anything in the mouth and do not try to hold the person down.
- Stay with the person until they are fully alert.
Call emergency help if the seizure lasts more than five minutes, another seizure begins immediately, the person is injured, or it is their first seizure.
What Is the Difference Between a Seizure and Epilepsy?
A seizure is an event, while Epilepsy is a condition that causes repeated seizures. For more information, please check the table below.
| Feature | Seizure | Epilepsy |
|---|---|---|
| Definition | A sudden burst of abnormal electrical activity in the brain | A long-term brain condition causing repeated seizures |
| Nature | Single event | Ongoing disorder |
| Frequency | May happen once | Happens repeatedly |
| Cause | Can be triggered by fever, low blood sugar, stress, or head injury | Usually diagnosed after two or more unprovoked seizures |
| Duration | Usually lasts seconds to a few minutes | A lifelong condition that needs management |
| Diagnosis | Based on one episode and medical tests | Diagnosed after repeated unprovoked seizures |
| Treatment | May not require long-term medication | Often requires regular anti-seizure medication |
| Example | A child having a seizure during a high fever | A person having seizures multiple times without fever or injury |
Types of Epileptic Seizures
Before reading this table, it is important to understand a simple difference. Seizure types describe what happens during a seizure — such as shaking, staring, or sudden jerking. These are based on how the brain activity spreads (focal or generalized).
On the other hand, epileptic seizure types or epilepsy syndromes are broader conditions. They include patterns of seizure types, age of onset, electroencephalogram(EEG) findings, causes, and long-term prognosis.
In simple words, a seizure type explains the event, while an epilepsy syndrome explains the overall condition. This section focuses only on the types of epileptic seizures, so you can clearly understand the symptoms without confusing them with epilepsy syndromes.
| Syndrome Name | Typical Age of Onset | Main Seizure Types | Key Symptoms / Features | Common Triggers | Stress Connection | Long-Term Outlook |
|---|---|---|---|---|---|---|
| Childhood Absence Epilepsy | 4–10 years | Absence seizures (staring spells) | Brief staring, pause in activity, no memory of the event, may happen many times daily | Fatigue, hyperventilation | Stress and emotional fatigue may increase episodes | Often outgrown with treatment |
| Juvenile Myoclonic Epilepsy (JME) | Teens (12–18 years) | Myoclonic jerks, tonic-clonic seizures | Sudden jerks (especially in the morning), possible full-body seizures | Sleep deprivation, alcohol | Stress and lack of sleep strongly increase seizures | Usually lifelong, but controlled with medicine |
| Lennox-Gastaut Syndrome | Early childhood (3–5 years) | Tonic, atonic, atypical absence | Multiple seizure types, learning difficulties, and developmental delay | Illness, sleep loss | Stress may worsen seizure control, but not cause it | Often difficult to control |
| Temporal Lobe Epilepsy | Late childhood or adulthood | Focal seizures | Unusual smells, sudden fear, confusion, repetitive movements, memory gaps | Emotional stress, lack of sleep | Emotional stress is a common trigger | May require long-term treatment |
| West Syndrome (Infantile Spasms) | Infancy (before 1 year) | Infantile spasms | Sudden body spasms in clusters, delayed development | Brain development issues | Not directly related to stress | Early treatment improves outcome |
| Dravet Syndrome | Infancy (first year of life) | Prolonged seizures, febrile seizures | Seizures triggered by fever, developmental delay | Fever, infections | Fever is the main trigger, not emotional stress | Requires lifelong specialized care |
Quick Summary of Key Differences
- Childhood Absence Epilepsy mainly causes short staring spells.
- JME causes morning jerks and is highly linked to sleep deprivation.
- Lennox-Gastaut Syndrome involves multiple seizure types and learning issues.
- Temporal Lobe Epilepsy often includes emotional symptoms like sudden fear.
- West Syndrome appears in babies and affects development.
- Dravet Syndrome is genetic and strongly linked to fever-triggered seizures.
Knowing the exact syndrome helps doctors choose the right treatment. Each syndrome has different triggers, age patterns, and long-term outlook.
7 Common Seizure Triggers
Seizures do not always happen without warning. In many people, certain factors increase the chance of a seizure. These are called seizure triggers. A trigger does not cause epilepsy, but it can make the brain more likely to have abnormal electrical activity. Knowing your personal triggers is one of the most powerful ways to prevent seizures.
Here are the 7 most common seizure triggers explained in simple terms:
1. Stress
Emotional stress is one of the most reported seizure triggers. When you feel stressed, your body releases hormones like cortisol and adrenaline. These chemicals increase brain activity and may lower the seizure threshold.
Common stress sources:
- Exams
- Work pressure
- Family conflict
- Anxiety
You can also monitor your stress using a stress level checker to better understand triggers that may increase seizure risk.
2. Lack of Sleep
Sleep deprivation is a strong trigger, especially in conditions like Juvenile Myoclonic Epilepsy.
When you don’t sleep enough:
- Brain activity becomes unstable
- Stress hormones increase
- Seizure threshold lowers
3. Missed Medication
Skipping anti-seizure medicine is a major risk factor. These medicines keep brain activity stable. Missing doses can quickly increase seizure risk.
4. Fever or Infection
High fever, especially in children, can trigger febrile seizures. Brain infections such as meningitis or encephalitis can also cause seizures.
5. Flashing Lights (Photosensitivity)
Some people are sensitive to flashing or flickering lights. This is called photosensitive epilepsy.
Possible triggers:
- Video games
- Strobe lights
- Rapid screen flashes
6. Alcohol or Drug Use
Alcohol affects brain chemicals. Drinking heavily or suddenly stopping alcohol can trigger seizures. Certain recreational drugs also increase risk.
7. Hormonal Changes
Hormonal shifts, especially in women, can influence seizure frequency. Some women experience more seizures during certain phases of the menstrual cycle. This is called catamenial epilepsy.
Can Seizures Cause Other Health Problems?
Seizures primarily affect the brain, but they can also affect other parts of the body. Many people worry about fever, memory problems, or heart issues after a seizure. In most cases, seizures are short and do not cause long-term health damage. However, depending on the type and duration, temporary effects can occur.
Can Seizure Cause Fever?

Seizures usually do not cause fever. In children, fever often triggers seizures (febrile seizures). Intense seizures may slightly increase body temperature due to muscle activity, but this effect is mild and transient. If a high fever occurs after a seizure, doctors check for infection, dehydration, or other illnesses.
Can a Seizure Cause Memory Loss?
Yes, seizures can cause temporary memory loss.
Memory gaps may happen before, during, or after a seizure:
- Before: Aura may not be remembered
- During: No awareness of the event
- After: Confusion during the postictal phase
During recovery, a person may experience confusion, trouble speaking clearly, and difficulty remembering recent events. Memory usually returns within minutes to hours.
Frequent seizures, especially in temporal lobe epilepsy, can affect long-term memory. Proper seizure control helps reduce this risk.
Can Seizures Cause Heart Problems?

Seizures can temporarily affect the heart rhythm.
During a seizure, a person may experience:
- Fast heartbeat (tachycardia)
- Slow heartbeat (bradycardia)
- Irregular heart rhythm
These changes usually return to normal once the seizure ends. Serious heart complications are rare, but in very rare cases, severe rhythm disturbances can occur.
A rare condition called SUDEP (Sudden Unexpected Death in Epilepsy) may involve breathing and heart rhythm problems after seizures. People with existing heart conditions should have regular medical monitoring.
Can a Seizure Cause Brain Damage?
Most seizures do not cause brain damage.
Short seizures (under 5 minutes) are usually harmless, as the brain can recover after brief abnormal electrical activity.
Temporary post-seizure symptoms may include:
- Confusion
- Memory gaps
- Headache
- Tiredness
- Difficulty concentrating
These symptoms are part of the postictal recovery phase and usually improve within a few hours.
When Can Brain Damage Happen?
- Risk increases if a seizure lasts more than 5 minutes (status epilepticus).
- Repeated seizures without regaining consciousness can be dangerous.
- Severe lack of oxygen during a seizure may harm brain cells.
- Untreated prolonged seizures in infants or the elderly carry a higher risk.
- Serious underlying brain conditions increase complications.
During long seizures, brain cells may become stressed due to:
- Reduced oxygen supply
- High energy demand
- Continuous abnormal electrical activity.
Do Frequent Seizures Cause Brain Damage?
Very frequent and uncontrolled seizures over time may affect:
- Memory
- Learning ability
- Thinking skills
This risk is higher in conditions like temporal lobe epilepsy. Proper treatment and regular medication greatly reduce long-term risk.
Diagnosis of Seizure
Diagnosing a seizure is the first step toward effective treatment. Doctors rely on a combination of medical history, eyewitness accounts, and diagnostic tests to confirm what type of seizure occurred and why. Early diagnosis helps prevent complications and guides proper management.
How to Detect Seizure Medically
Doctors use several medical tests to detect seizures and understand their cause. Each method helps examine brain activity or identify health problems that may trigger seizures.
Electroencephalogram (EEG)

An EEG measures the electrical activity of the brain. Small sensors are placed on the scalp to record brain signals. If seizures occur, the test may show abnormal electrical patterns that help doctors confirm the diagnosis.
MRI (Magnetic Resonance Imaging)

An MRI scan produces detailed images of the brain. It helps doctors detect structural problems such as tumors, scar tissue, brain injuries, or abnormal brain development that could cause seizures.
CT Scan (Computed Tomography)
A CT scan uses X-rays to create images of the brain. Doctors often use it in emergencies to check for brain bleeding, swelling, or head injuries that might trigger seizures.
Blood Tests
Blood tests help identify medical conditions that may lead to seizures. These tests check for infections, low blood sugar, electrolyte imbalance, or other metabolic problems.
Video EEG Monitoring
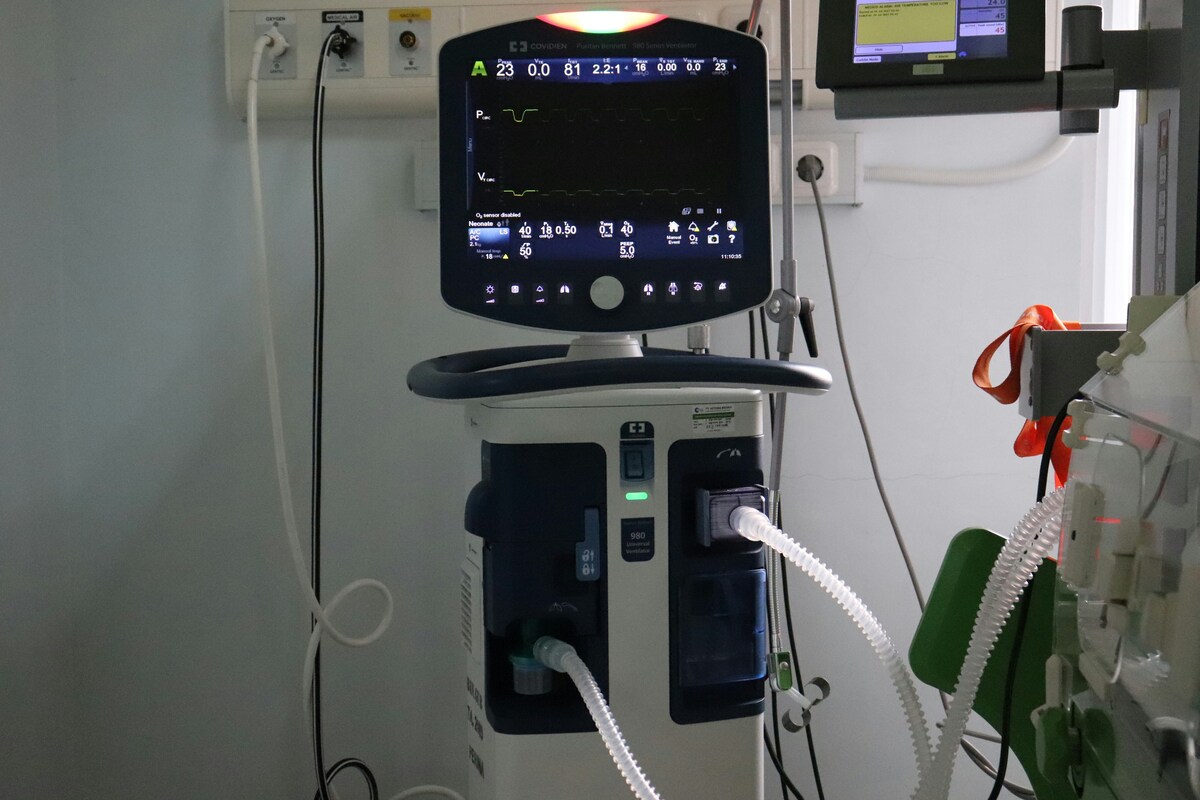
Video EEG combines brain wave recording with video monitoring. The patient stays under observation while both brain activity and body movements are recorded. This helps doctors clearly see what happens during a seizure and make an accurate diagnosis.
Guidelines for the Treatment of Seizures
Seizure and epilepsy disorders are neurological conditions that need proper medical treatment and regular monitoring. Treatment usually includes anti-seizure medications, healthy lifestyle habits, and in some cases, specialized therapies to control symptoms and improve quality of life.
1. Seizure Medicines (Anti-Epileptic Drugs)
Anti-epileptic Drugs (AEDs)
Anti-epileptic drugs are the main treatment used to control seizures. These medicines work by stabilizing brain activity and reducing abnormal electrical signals that lead to seizures.
When taken regularly, these medications help reduce how often seizures happen and how severe they are. For many patients, proper medication allows them to live a normal and active life.
Common Medications
Doctors commonly prescribe medicines such as Valproate (Valproic Acid), Carbamazepine, Lamotrigine, Levetiracetam, and Phenytoin. Each drug works differently, so the choice depends on the patient’s condition.
2. Therapies Used for Seizure and Epilepsy Disorders

Seizure and epilepsy treatment may involve more than just medication. In some cases, doctors recommend special diets, medical devices, surgery, or psychological support to help control seizures. These therapies are usually considered when seizures are frequent or do not respond well to standard medications.
Ketogenic Diet Therapy

The ketogenic diet is a high-fat and very low-carbohydrate diet that helps reduce seizures, especially in children who do not respond well to medications. A calorie calculator can help manage daily calorie intake while following this diet. Maintaining a healthy weight with the help of a BMI calculator can also support long-term well-being.
Vagus Nerve Stimulation (VNS)
Vagus nerve stimulation uses a small device placed under the skin in the chest. The device sends mild electrical signals to the brain through the vagus nerve, which may help reduce seizure frequency.
Responsive Neurostimulation (RNS)

Responsive neurostimulation involves a device implanted in the brain. It monitors brain activity and delivers small electrical signals when abnormal patterns appear. This can help stop seizures before they fully develop.
Epilepsy Surgery
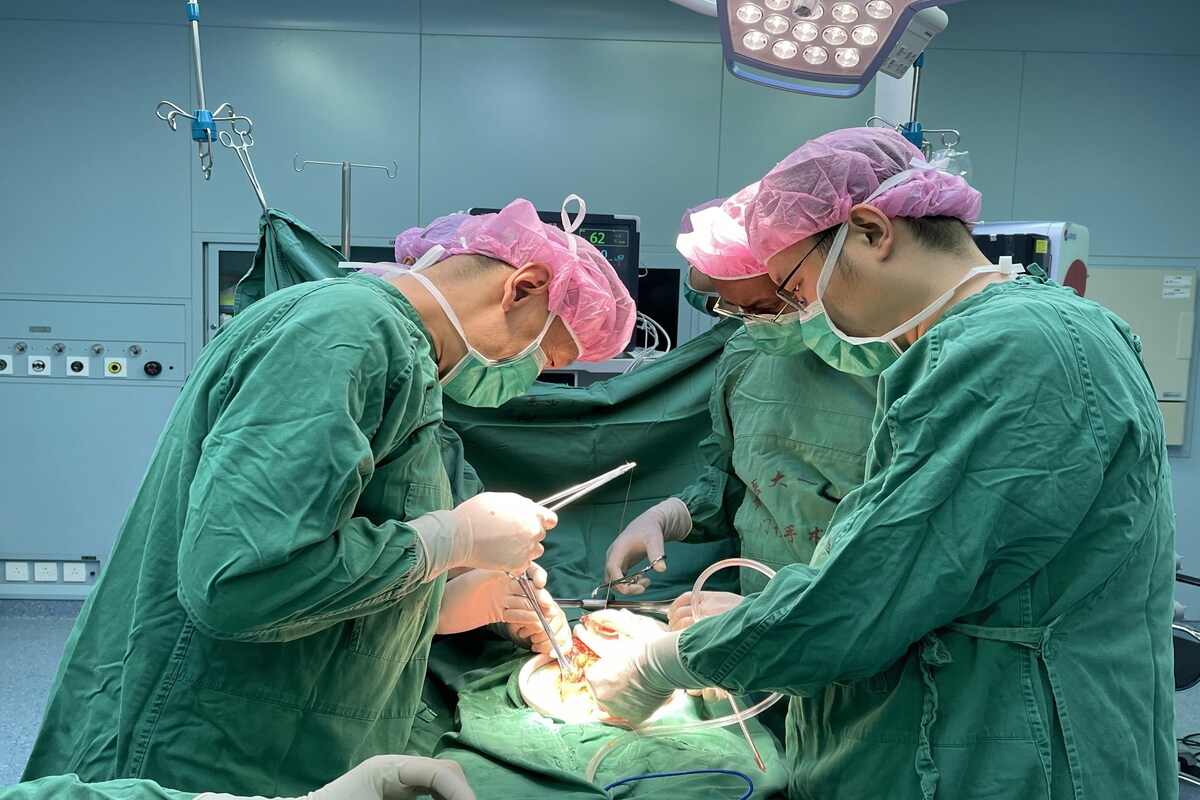
Surgery may be recommended when seizures start from a specific part of the brain and medicines are not effective. The goal is to remove or disconnect the area causing the seizures.
Behavioral or Psychological Therapy
Psychological support can help people manage stress and emotional triggers. Techniques such as counseling, relaxation, and stress management may reduce seizure episodes in some individuals.
Treatment plans are personalized and supervised by a neurologist.
Risks and Complications of Epileptic Seizures
Epileptic seizures can sometimes lead to health risks if they occur frequently or remain uncontrolled. These complications may affect physical safety, brain function, and emotional well-being.
- Physical Injuries – Seizures can cause sudden loss of control, which may lead to falls, burns, or other accidents.
- Status Epilepticus – This is a seizure that lasts longer than a few minutes or repeated seizures without recovery. It is a serious medical emergency.
- Concentration Issues – Some people experience difficulty focusing on daily tasks, studies, or work after seizures.
- Emotional Challenges – Living with seizures can increase the risk of anxiety, depression, and mood changes.
- Sudden Unexpected Death in Epilepsy (SUDEP) – This is a rare but serious complication in people with epilepsy where sudden death occurs without a clear cause.
Proper treatment and regular medical care can help reduce these risks.
FAQs
1. Can you have a seizure from stress without epilepsy?
Yes, severe stress can trigger seizure-like episodes in some people, even without epilepsy. These are often called psychogenic nonepileptic seizures (PNES).
2. What autoimmune disease can cause seizures?
Autoimmune conditions such as lupus, autoimmune encephalitis, and multiple sclerosis can affect the brain and may lead to seizures.
3. What happens if you leave seizures untreated?
Untreated seizures can become more frequent and severe. They may also increase the risk of injury, memory problems, and serious complications.
4. Can you be hospitalized for a seizure?
Yes, hospitalization may be required if the seizure lasts too long, repeats frequently, causes injury, or happens for the first time.
5. What does the ER do for seizures?
Emergency doctors monitor breathing and heart rate, stop the seizure with medication if needed, and perform tests to identify the cause.
6. What are the 3 C’s for seizures?
The 3 C’s are Stay Calm, Cushion the head, and Call for help if the seizure lasts too long or the person is injured.
7. Which part of the brain is removed for seizures?
In some cases, doctors remove the small area of the brain where seizures start, often in the temporal lobe.
8. How to spot fake seizures?
Psychogenic nonepileptic seizures may look different from epileptic seizures. Diagnosis requires medical evaluation with tests such as video EEG monitoring.
9. Which food triggers seizures?
Some people may have seizures triggered by caffeine, alcohol, artificial sweeteners, or foods that cause blood sugar changes. Triggers vary from person to person.
10. Can seizures cause elevated troponin?
Yes, in some cases, seizures can temporarily raise troponin levels due to stress on the heart during the episode.
11. Can overthinking cause seizures?
Overthinking alone usually does not cause seizures, but severe stress and anxiety may trigger seizures in people who are already vulnerable.
12. Can seizures come on suddenly?
Yes, seizures can appear suddenly without warning. However, some people experience early signs such as unusual sensations, mood changes, or dizziness before a seizure begins.
Conclusion
Conclusion
Understanding Can Stress Cause Seizures is important for both patients and caregivers. While stress alone does not usually cause epilepsy, it can act as a powerful trigger in people who are already vulnerable.
The good news is that seizures can often be managed effectively with the right treatment and lifestyle choices. Early diagnosis, proper medication, balanced nutrition, good sleep, and stress management all play a key role in reducing seizure frequency and improving quality of life.
Learning to recognize seizure symptoms, understanding seizure triggers, and following medical advice can help people stay safer and more in control of their health. With proper care, support, and awareness, many individuals with seizures or epilepsy are able to live active, healthy, and fulfilling lives.
Note: This article is for informational and educational purposes only. It does not replace professional medical advice. If you experience seizures, severe stress, or other health concerns, consult a qualified healthcare professional for proper diagnosis and treatment.

