Gout is a painful inflammatory form of arthritis caused by the accumulation of uric acid crystals inside joints. These microscopic crystals develop when uric acid levels in the bloodstream become too high, a condition known medically as hyperuricemia. When these crystals settle into joints, the immune system reacts strongly, leading to swelling, redness, warmth, and intense pain. Many people describe their first gout attack as sudden and shocking—often occurring overnight and making it difficult to even touch the affected joint. Stress and gout are closely linked, as high stress levels can trigger flare-ups or worsen symptoms in susceptible individuals. Managing this is easier when you understand how exercise and stress management can lower your body’s inflammatory response.
Research published in global rheumatology studies suggests that around 3–4% of adults worldwide experience gout, and the numbers are rising due to modern lifestyle factors such as obesity, processed diets, and sedentary habits. While gout is commonly associated with the big toe, it can also affect the knees, ankles, fingers, and other joints.
From a biological perspective, gout develops when the body struggles to manage purines properly. Purines are natural chemical compounds found in many foods and also produced during normal cell turnover.
Lifestyle plays a major role in this process. Weight gain and metabolic disorders also contribute to higher uric acid levels. Many health professionals recommend monitoring overall wellness indicators to reduce risk. For example, using a BMI calculator can help individuals determine whether body weight might be contributing to elevated uric acid levels.
How Uric Acid Builds Up in the Body
To fully understand gout symptoms, it helps to explore the underlying metabolic process behind the disease. Uric acid is created when the body breaks down purines found in both food and human cells. Normally, this substance dissolves in the bloodstream and travels to the kidneys, where it is filtered and eliminated through urine. The body maintains a delicate balance between uric acid production and removal.
When Uric Acid Removal Slows Down
Trouble begins when that balance is disrupted. Some people naturally produce more uric acid due to genetic factors, while others experience reduced kidney efficiency that slows the removal process. When uric acid accumulates, it can crystallize and deposit in joints. These crystals have sharp edges that irritate joint tissues and trigger intense inflammation.
The Role of Diet in Uric Acid Production

Diet plays a surprisingly strong role in this mechanism. Foods such as organ meats, shellfish, red meat, sugary drinks, and alcohol contain high purine levels. Consuming them regularly can increase uric acid production. Alcohol can also interfere with kidney filtration, making it harder for the body to remove uric acid effectively.
Why Hydration Matters for Uric Acid Removal

Hydration is another key factor. When someone drinks insufficient water throughout the day, urine becomes concentrated, and kidney function becomes less efficient. Adequate hydration helps flush excess uric acid from the body and reduce the risk of crystal formation.
Body Weight and Uric Acid Levels

Weight management is equally important. Studies consistently show that individuals with higher body weight have higher uric acid levels because excess adipose tissue influences metabolic pathways. This is why doctors frequently recommend lifestyle tools such as a calorie calculator to help individuals manage their daily food intake and maintain a balanced diet.
Connection between Stress and Gout Flare-Ups
Stress can also play a subtle role. Chronic stress alters hormone levels and inflammatory responses in the body. Some patients notice that gout flare-ups appear during stressful periods such as work deadlines or major life changes. Monitoring emotional health using a stress level checker can sometimes reveal patterns between stress and gout attacks.
Think of uric acid metabolism like a sink with a faucet and a drain. If the faucet produces water faster than the drain can remove it, the sink eventually overflows. In gout, the faucet represents uric acid production, and the drain represents renal clearance. When production exceeds elimination, crystals begin to form, leading to painful gout symptoms.
Symptoms of Gout
Gout is a type of inflammatory arthritis that occurs when uric acid crystals accumulate in the joints, triggering sudden pain, swelling, and inflammation. Unlike many chronic conditions, gout attacks appear suddenly and intensely, often at night or early morning. Early recognition of these symptoms is important to prevent long-term joint damage and preserve mobility.
General Symptoms of Gout
- Sudden, intense pain in one or more joints.
- Swelling and redness, making the joint appear puffy.
- Warmth and tenderness; even a light touch, such as a bedsheet brushing the joint, can be painful.
- Stiffness and reduced range of motion, which can make walking or other movements difficult.
- Some people may experience mild fever, fatigue, or general discomfort during severe attacks. You can use a stress level checker to see if your physical exhaustion is being worsened by mental pressure.
- A typical attack lasts 3 days to 2 weeks. Early attacks may occur infrequently, but without proper management, attacks often become more frequent.
Acute vs. Chronic Gout
- Acute gout occurs suddenly with severe pain, usually in a single joint.
- Chronic gout develops over time due to persistent uric acid buildup, often affecting multiple joints and leading to tophi (visible lumps of urate crystals under the skin). Chronic gout can cause ongoing joint stiffness, reduced mobility, and more frequent flare-ups. Engaging in a low-impact exercise routine can help keep joints flexible without overstraining them.
Joint-Specific Symptoms
Feet and Big Toe (Podagra):

- The most common site for gout attacks is the big toe joint (first metatarsophalangeal joint).
- Suddenly, sharp pain often starts at night.
- Swelling, redness, and shiny or tight skin; sometimes peeling or itching as the attack heals.
- Throbbing or burning sensations and extreme tenderness make walking or wearing shoes difficult.
- Repeated attacks can cause stiffness and limited movement over time.
Knee Gout:
- Pain worsens with bending or standing.
- Swelling and stiffness can limit movement; the knee may appear visibly enlarged due to fluid buildup.
- Warmth and redness around the joint are common.
- Daily activities like climbing stairs, kneeling, or standing from a chair become difficult.
Hands and Finger Joints:
- Swelling, stiffness, and pain can interfere with daily tasks such as typing, writing, or gripping objects.
- Nodules or tophi may appear in chronic cases.
- Early treatment helps preserve hand mobility and prevent long-term damage.
Ankle Gout:
- Causes swelling, redness, and warmth in the joint.
- Walking and bearing weight can become painful even with mild inflammation.
- May result in stiffness and difficulty performing normal movements.
Other Joints (Wrists, Elbows, Shoulders):
- Pain, swelling, and limited mobility can affect daily activities.
- Chronic attacks may lead to tophi formation around these joints.
What Are the Stages of Gout?
Gout usually develops gradually and progresses through four main stages. Understanding these stages can help people recognize early warning signs and seek treatment before the condition becomes more severe.
1. Asymptomatic Hyperuricemia
This is the earliest stage of gout. At this stage, uric acid levels in the blood are higher than normal, but there are no visible symptoms yet. Although a person may not feel pain, uric acid crystals can begin forming in the joints. Many people remain in this stage for years before experiencing their first gout attack. Using a BMI calculator can help you manage weight-related risks before the first painful attack occurs.
2. Acute Gout Attack
This stage occurs when uric acid crystals trigger sudden inflammation in a joint. It often causes severe pain, redness, swelling, and warmth, usually in the big toe but sometimes in the knee, ankle, or other joints. Acute gout attacks commonly start at night or early in the morning and may last several days.
3. Intercritical Gout (Symptom-Free Period)
After an acute attack subsides, gout enters a stage called intercritical gout, which is the period between flare-ups. During this time, symptoms disappear, and the person may feel normal again. However, uric acid crystals may still remain in the joints, which means future attacks can occur if the condition is not managed properly.
4. Chronic Tophaceous Gout
This is the most advanced stage and usually develops after many years of untreated or poorly controlled gout. In this stage, urate crystals accumulate and form lumps called tophi under the skin around joints. Chronic gout can lead to persistent pain, joint damage, and reduced mobility if not treated effectively.
Possible Causes of Gout
Elevated uric acid levels can lead to gout, with causes ranging from stress and diet to kidney function and inherited traits, making some individuals more susceptible than others.
1. Stress and Lifestyle Triggers
Stress is a major factor that can trigger or worsen gout attacks. Both physical and emotional stress increase inflammation in the body and can affect how uric acid is processed. Chronic emotional stress doesn’t just trigger gout; in extreme cases, it can also lead to neurological issues. Many people ask, Can stress cause seizures?, and the answer lies in how our nervous system handles intense pressure. Common triggers include:
- Emotional stress from work pressure, anxiety, or personal challenges.
- Physical stress such as illness, surgery, or intense exercise.
- Sleep deprivation or sudden lifestyle changes can disturb uric acid balance.
Even in individuals with controlled uric acid levels, these stressors can provoke sudden gout flare-ups. Managing stress through relaxation techniques, adequate sleep, and balanced routines is an important part of gout prevention.
2. Excess Uric Acid Production
The body produces uric acid when it breaks down purines, compounds found in certain foods and drinks. Overproduction can overwhelm the kidneys’ ability to eliminate it, leading to urate crystal formation in the joints.
3. Poor Kidney Function
Kidneys help remove uric acid from the body through urine. If kidney function is impaired, uric acid can accumulate, increasing the risk of gout attacks.
4. Diet High in Purines
Foods rich in purines can raise uric acid levels, including red meat, organ meats, seafood (sardines, anchovies, shellfish), and sugary drinks. Alcohol, especially beer and spirits, is also a common contributor. Managing your daily intake with a calorie calculator can help you maintain a gout-friendly diet.
5. Obesity and Metabolic Conditions
Being overweight increases the risk of hyperuricemia and gout. Conditions such as high blood pressure, diabetes, and high cholesterol are linked to a higher likelihood of developing gout.
6. Genetics and Family History
A family history of gout can increase your risk, as certain genes affect how the body processes uric acid.
7. Medications and Medical Conditions
Some medications, such as diuretics, low-dose aspirin, and immunosuppressants, can raise uric acid levels. Medical conditions like kidney disease, hypothyroidism, and certain cancers may also contribute.
8. Age and Gender Factors
Gout is more common in men over 30 and postmenopausal women, due to hormonal differences that influence uric acid levels.
How Doctors Diagnose Gout and the Role of Stress
Diagnosing gout involves a combination of medical history, physical examination, and diagnostic tests. Because gout symptoms can sometimes resemble other types of arthritis, doctors use several methods to confirm the condition and rule out similar joint disorders. Early and accurate diagnosis is important for starting the right treatment and preventing long-term joint damage.
1. Medical History and Symptom Review
The first step in diagnosing gout is discussing your symptoms and medical history. Doctors typically ask when the pain started, how severe it is, and whether the attacks occur suddenly—often at night. They may also ask about your diet, alcohol intake, family history of gout, and existing health conditions such as kidney disease or high blood pressure. This information helps identify possible triggers and risk factors.
2. Physical Examination
During a physical exam, the doctor carefully examines the affected joint. Signs such as swelling, redness, warmth, and tenderness can indicate gout. The doctor may also check for tophi, which are small lumps of urate crystals that can develop under the skin in long-term cases.
3. Joint Fluid Test (Synovial Fluid Analysis)
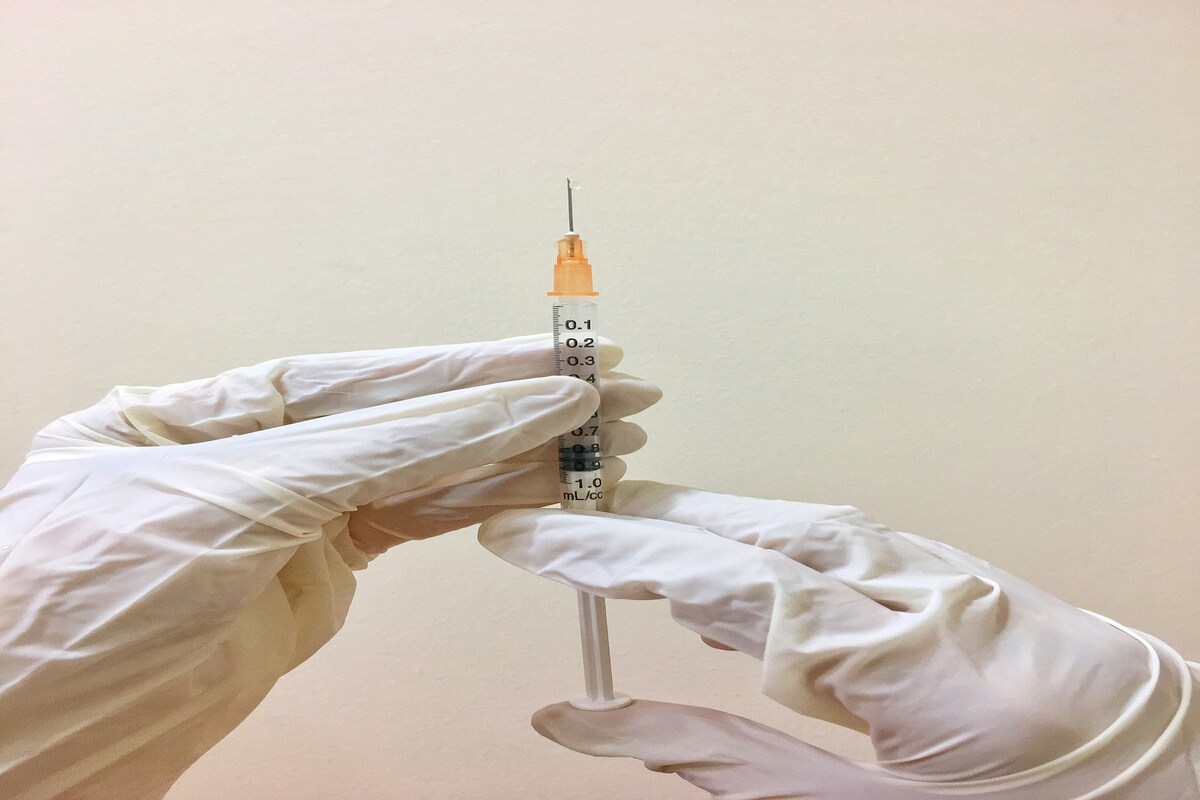
One of the most reliable ways to diagnose gout is by examining fluid taken from the affected joint. In this test, the doctor uses a thin needle to remove a small sample of joint fluid. The fluid is then analyzed under a microscope to look for uric acid crystals, which confirm the presence of gout.
4. Blood Tests
Blood tests may be used to measure the level of uric acid in the bloodstream. High uric acid levels can support a diagnosis of gout, although it is important to note that some people with elevated levels never develop gout, while others may have normal levels during an attack.
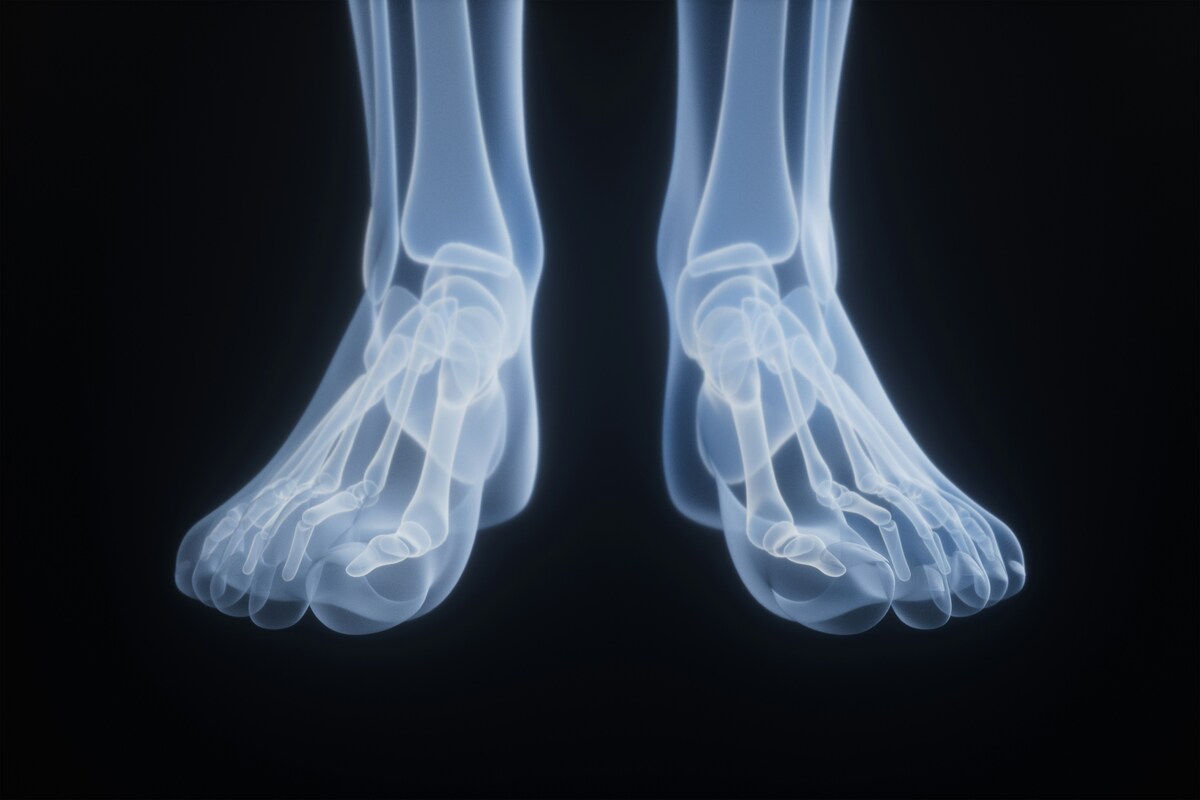
5. Imaging Tests
Imaging techniques can help doctors see joint damage or crystal deposits. These tests may include:
- X-rays, which help rule out other causes of joint pain.
- Ultrasound, which can detect uric acid crystal deposits in joints and surrounding tissues.
- Dual-energy CT scans, which can clearly identify urate crystal buildup in the body.
6. Ruling Out Other Conditions
Because gout symptoms can resemble other types of arthritis, doctors may also check for conditions such as rheumatoid arthritis, osteoarthritis, or joint infections. Proper diagnosis ensures that the correct treatment plan is used.
Accurate diagnosis allows doctors to develop an effective treatment plan to reduce pain, control inflammation, and prevent future gout attacks. Early medical evaluation is especially important for people who experience sudden, severe joint pain or recurring flare-ups.
What Happens If Gout Goes Untreated
If gout is not properly treated, the condition can gradually worsen and lead to serious joint and health problems. While early gout attacks may occur occasionally and resolve on their own, untreated gout often becomes more frequent, longer-lasting, and more severe over time. Continuous uric acid buildup can cause permanent damage to joints and surrounding tissues.
1. More Frequent and Severe Attacks
Without treatment, gout attacks may occur more often and last longer. What initially starts as occasional flare-ups can eventually become chronic and persistent, affecting multiple joints and causing ongoing pain.
2. Chronic Joint Damage
Repeated inflammation can gradually damage cartilage and bone within the joint. Over time, this damage may lead to permanent stiffness, reduced mobility, and deformity in the affected joints.
3. Formation of Tophi
In advanced cases, deposits of uric acid crystals can accumulate under the skin and form hard lumps called tophi. These lumps often appear around joints, fingers, toes, elbows, or ears and may interfere with normal joint function.
4. Kidney Problems
High uric acid levels can also affect the kidneys. Untreated gout may increase the risk of kidney stones or reduced kidney function, which can further worsen uric acid buildup in the body.
5. Reduced Quality of Life
Persistent pain, swelling, and limited joint movement can make daily activities such as walking, working, or exercising more difficult. Over time, untreated gout may significantly impact mobility, independence, and overall quality of life.
Treatment of Gout Disease
The treatment of gout focuses on relieving pain during flare-ups, reducing inflammation, lowering uric acid levels, and preventing future attacks. Doctors usually combine medications, lifestyle changes, and long-term management strategies to control the condition and protect joint health.
1. Medications for Acute Gout Attacks
During a gout flare-up, treatment aims to quickly reduce pain and inflammation. Common medications include:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Medicines such as ibuprofen or naproxen help relieve pain and reduce swelling.
- Colchicine: A medication that reduces inflammation caused by uric acid crystals, especially when taken early in an attack.
- Corticosteroids: These may be taken orally or injected into the affected joint to control severe inflammation when other drugs are not suitable.
2. Medications to Lower Uric Acid Levels
For people with frequent attacks or chronic gout, doctors may prescribe long-term medications to reduce uric acid levels and prevent crystal formation. These include:
- Xanthine oxidase inhibitors: These medications reduce the body’s production of uric acid.
- Uricosuric drugs: They help the kidneys remove more uric acid through urine.
- Newer uric-acid–lowering therapies: In severe cases, specialized medications may be used to break down uric acid in the body.
3. Lifestyle and Dietary Changes
Lifestyle management is an essential part of gout treatment. Doctors often recommend:
- Maintaining a healthy body weight reduces stress on joints.
- Limiting foods high in purines, such as red meat, organ meats, and certain seafood.
- Reducing alcohol intake, especially beer and spirits.
- Avoiding sugary drinks and high-fructose foods.
- Drinking plenty of water helps flush uric acid from the body.
4. Home Care During Gout Attacks
Certain self-care measures can help reduce discomfort during flare-ups:
- Rest the affected joint and avoid pressure on it.
- Applying cold packs or ice to reduce swelling and pain.
- Keeping the joint elevated to reduce inflammation.
- Wearing loose and comfortable footwear if the foot is affected.
5. Stress Management and Lifestyle Balance
Managing stress and maintaining a balanced lifestyle can play an important role in controlling gout. Physical or emotional stress can trigger inflammation in the body, which may contribute to gout flare-ups.
Regular moderate exercise, such as walking, stretching, or yoga, can help improve circulation and support overall joint health. Practicing relaxation techniques, including deep breathing, meditation, or mindfulness, may also help lower stress levels and reduce inflammation in the body.
Getting adequate rest, staying hydrated, and following a balanced daily routine can support better overall health and help reduce the frequency of gout flare-ups.
6. Treatment of Underlying Conditions
Managing related health conditions can also improve gout control. Doctors may monitor and treat issues such as high blood pressure, kidney disease, obesity, and metabolic syndrome, which are often linked to gout.
7. Surgical Treatment in Severe Cases
Surgery is rarely needed but may be considered when gout leads to large tophi deposits, severe joint damage, or chronic pain. Surgical removal of tophi or joint repair procedures may help restore function in advanced cases.
With proper treatment and long-term management, most people with gout can control symptoms, reduce the frequency of attacks, and maintain good joint health.
Gout treatment focuses on reducing pain during attacks and lowering uric acid levels to prevent future episodes. Lifestyle changes often play a major role alongside medication.
Maintaining a healthy weight, improving diet, staying hydrated, and managing stress can significantly reduce flare-ups.
Frequently Asked Questions About Stress and Gout
1. Which vegetables may help lower uric acid levels?
Certain vegetables can support healthy uric acid levels, especially those rich in antioxidants and fiber. Vegetables such as spinach, broccoli, cucumbers, celery, and carrots may help the body process uric acid more efficiently. A balanced diet that includes plenty of vegetables can also reduce inflammation associated with gout.
2. What drinks can help flush out uric acid?
Drinking enough fluids can help the kidneys remove excess uric acid. Water is the most effective option, but beverages like lemon water, green tea, and cherry juice may also help reduce inflammation and support uric acid balance.
3. When are uric acid levels usually highest during the day?
Uric acid levels are often highest in the early morning hours. This is partly because the body becomes slightly dehydrated during sleep, and metabolic processes overnight can lead to higher concentrations of uric acid.
4. Is it possible to permanently reduce uric acid levels?
While uric acid cannot always be eliminated permanently, it can be effectively controlled. Lifestyle changes, a balanced diet, proper hydration, stress management, and prescribed medications can help maintain healthy uric acid levels and prevent gout attacks.
5. Can people with lower incomes develop gout?
Yes, gout can affect people from any economic background. However, diet, access to healthcare, lifestyle habits, and underlying health conditions may influence the risk of developing gout.
6. Can fasting trigger a gout attack?
In some cases, prolonged fasting or extreme dieting may increase the risk of gout flare-ups. When the body breaks down stored fat rapidly, uric acid levels may rise, which can trigger inflammation in the joints.
7. Is it possible to build muscle if you have gout?
Yes, people with gout can still build muscle safely. The key is to follow a balanced exercise routine, stay hydrated, avoid excessive high-purine foods, and manage stress levels that could trigger flare-ups.
8. Does sweating help with gout?
Sweating alone does not remove large amounts of uric acid. However, regular physical activity that causes mild sweating can improve overall health, support metabolism, and help maintain a healthy weight, which may reduce gout risk.
9. Should I take vitamin B12 if I have gout?
Vitamin B12 is generally safe for people with gout and may support nerve health and energy levels. However, supplements should only be taken after consulting a healthcare professional, especially if you already take medications.
10. Is applying ice helpful during a gout attack?
Yes, applying ice packs to the affected joint may help reduce swelling and numb pain during a gout flare-up. It is usually recommended to apply ice for 10–15 minutes at a time.
11. Can massage therapy help gout pain?
A gentle massage around the affected area may improve blood circulation and reduce muscle tension. However, direct massage on an inflamed gout joint should be avoided during an active attack because it may worsen pain.
Conclusion
Gout can be a painful and disruptive condition, but understanding its early symptoms, causes, and stages can make a significant difference in managing it effectively. By recognizing the warning signs early and seeking proper medical guidance, many people can prevent severe flare-ups and protect their joint health. It is also important to understand the connection between stress and gout, as high stress levels may trigger or worsen attacks in some individuals. Maintaining a balanced lifestyle, staying hydrated, following a healthy diet, and managing stress can all help reduce the risk of future episodes. With the right knowledge and preventive steps, people living with gout can take control of their condition and maintain a healthier, more active life.
Note: The information provided here is for informational purposes only. It is not a substitute for medical care. If you have frequent or intense gout flare-ups or any concerning symptoms, seek guidance from a licensed healthcare provider.
May you also read: Can Stress Cause Seizures?